LCPC Note: This blog post was the most viewed blog published on EAPC in 2022.
What matters most to patients and families at end of life: Findings from Quality of Death and Dying Index 2021
The Lien Centre for Palliative Care at Duke-NUS Medical School, commissioned by the Lien Foundation, has produced the Cross Country Comparison of Expert Assessments of the Quality of Death and Dying Index 2021. Professor Eric Finkelstein, Executive Director of Lien Centre for Palliative Care, Duke-NUS Medical School, Singapore and Duke Global Health Institute, Durham, North Carolina, US, explains.

Professor Eric Andrew Finkelstein
Note: This article has been duplicated with the permission of EAPC.
Over two years ago I was commissioned to lead a study that would rank countries on the ‘quality of death and dying’. This follows two similar studies conducted in 2010 and 2015 with a similar focus. Rather than replicate the approach taken by past studies, colleagues and I decided to take on a more innovative, yet riskier approach. Prior efforts largely focused on ranking countries based on factors thought to be correlated with a good end-of-life experience, such as the existence of a national strategy for palliative care and staffing ratios of health professionals. Although these metrics are readily available, it is unclear how well they correlate with delivering on what matters most to patients and families at end of life. Answering that question requires a better understanding of patient and caregiver preferences and a strategy to measure how well those preferences are met.
To meet that objective, we first undertook an extensive literature review to identify factors that patients, caregivers, and health professionals believe are important at end of life. We then used something called a discrete choice experiment (DCE) to measure the relative value of these factors. A DCE is a survey technique but basically acts like a game of ‘would you rather’. In this case, we provided 1,250 respondents across five countries with a series of end-of-life scenarios and asked which scenario they would prefer for a loved one with a life-limiting condition. By asking enough questions we were able to quantify not only what is perceived as most important at end of life, but the relative value of each factor compared to the others. What we found is detailed in the second publication and summarised below.
Relative Importance for Each End-of-Life Care Indicator
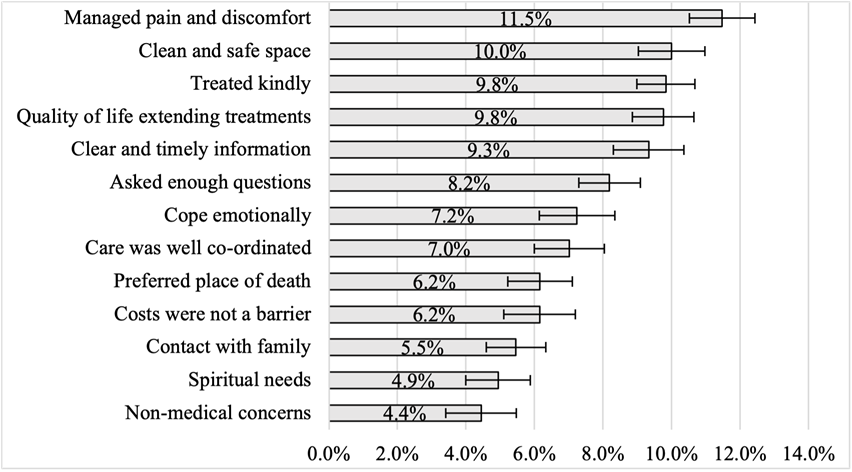
Note: Error bars indicate 95% Confidence intervals
As one might guess, managing pain and discomfort is the number one priority at end of life. However, what may be surprising is that respondents rank other factors, such as receiving care in clean and safe spaces, and being treated kindly only slighter lower on the list and similar to their assessment of the value of the quality of life-extending treatments. Factors that ranked lowest on the list were ensuring contact with family/friends and addressing spiritual needs and other non-medical concerns. However, as this survey was conducted before the surge in Covid-19 cases, it is possible that lack of experience with having loved ones die in isolation may have pushed this and related factors lower in the rankings. Regardless, these results show what both developed and developing countries can do to improve end-of-life care. Importantly, many of these areas can be improved without a significant outlay of resources. In fact, treating patients at home when possible and avoiding overtreatment could even save money, although that should certainly not be the focus of end-of-life care.
Cross Country Comparison of Expert Assessments of the Quality of Death and Dying 2021
With the completion of the above analysis we had an instrument with weighting factors that could be used to score countries (or regions, health systems, hospitals,…) on end-of-life care delivery. However, our next challenge was who to survey to get the results. We would have ideally liked to survey hundreds or even thousands of end-of-life patients or their caregivers in countries around the world, but this was simply not feasible with the time and resources available. We ultimately opted to survey key informants at the country level whom we felt could provide reasonable responses that would be correct on average. We had hoped to get input from many respondents in all countries but the high demands of Covid and other factors limited our ability to obtain timely feedback. In the end, our final ranking included input from at least two key informants from 79 countries (and Hong Kong and Taiwan), representing 81 per cent of the world’s population. You can see the full ranking and grades for the included countries here with additional information available on our website.
A starting point for future advocacy and research to improve end-of-life care
To me, the country-level ranking is less important than the stark difference in outcomes for higher-income countries compared to others. Five of the top six countries, those that received a grade of A, were high-income countries. At the other extreme, 21 countries received a failing grade and only two are high-income countries. This highlights the large disparities in the quality of end-of-life care across countries, especially between the highest-income countries and others.
Although our study is not perfect, we believe it represents a starting point for both future advocacy and research efforts and provides a clear strategy for what countries can do to improve their score and the end-of-life experience for patients and caregivers, which is our ultimate objective.