Fighting the pandemic with data
Healthcare workers at Singapore General Hospital underwent special training to ensure they could perform life-saving procedures smoothly while wearing full PPE // Credit: Singapore General Hospital
It was a Saturday night when Dr Ken Goh got the call.
“I remember rushing to the hospital to see a patient whose condition had deteriorated rapidly,” said Goh, an associate consultant with the Department of Respiratory and Critical Care Medicine at Singapore General Hospital (SGH).
The patient was the hospital’s first COVID-19 patient to need emergency intubation, a procedure whereby a tube is inserted into a patient’s airway to help them to breathe.
While the procedure is a standard one for severely ill patients, performing it in full personal protective equipment (PPE) while leaning over a patient with a highly contagious new virus was daunting. But as Goh stepped into the intensive care unit (ICU), any anxiety that he felt was gone.
“Strangely, it was easy to focus and maintain my composure once I had arrived,” said Goh, an alumnus of Duke-NUS (Class of 2012). “What helped was that the team shared a strong sense of duty to the patient and we trusted each other completely.”
As the first cases of human-to-human transmission emerged from Wuhan back in January, Goh and the ICU team knew that they had to be ready. They worked with colleagues from various hospital departments to adapt protocols and develop new training modules, so that they and their healthcare colleagues could continue to provide the best care for their patients safely. They organised simulation sessions, such as how to perform life-saving cardiopulmonary resuscitation while wearing PPE, so that the team could perform these drills smoothly.
In addition to preparing healthcare workers to handle the pandemic, Goh and the ICU team contributed to the hospital-wide effort to ensure that crucial medical equipment and consumables, ranging from ventilators to PPE and essential medication, were well stocked.
When the first cases were reported in Singapore, the ICU team was ready to face a surge in critically ill COVID-19 patients. While the numbers climbed steadily during the early months of the outbreak, they never outstripped the hospital’s capacity or overwhelmed the team.

A healthcare worker wearing PPE is about to enter the isolation ward // Credit: Singapore General Hospital
Rolling out a rapid response
Singapore’s preparations for a pandemic were an effective breakwater that slowed the spread of the virus.
“Singapore did well. We have very low mortality for the number of cases that we have had,” said Professor Marcus Ong, Director of the Duke-NUS Health Services and Systems Research (HSSR) Programme.
“It is a great achievement that we’ve been able to protect patients and insulate our healthcare system such that we have not been overwhelmed,” he added.
While preparedness allowed Singapore to mitigate the impact of this novel coronavirus, the age profile of those who were infected also played a part in the outcomes.
“What worked in our favour was the fact that while, on the one hand, we were ramping up our capabilities and resources, on the other hand, the newly infected population was younger and less likely to need intensive services,” said Professor David Matchar from the HSSR Programme.
Emerging stronger from previous battles
When SARS arrived on Singapore’s shores in 2003, it spread quickly. Among its chief casualties were members of the healthcare family.
Taking that to heart, hospitals and emergency departments across Singapore reviewed their operating procedures and invested in infectious disease preparedness. On a national level, Singapore also invested in a state-of-the-art national disease outbreak centre.
“We underwent a paradigm shift. Unlike in most countries, here, we routinely separate emergency patients into those who are ‘suspect’ infectious disease cases and those who are not,” said Ong, who is also a senior emergency physician at SGH. He added that the chain of isolation goes all the way from triage assessment to treatment area so that when patients who may have an infection see healthcare staff, the staff are already wearing the right PPE.
Even with fever screening as an existing part of the protocol, adjustments had to be made. The fever screening area had to be expanded and an additional process for confirmed COVID-19 patients was set up.

Professor Marcus Ong (left) and Professor David Matchar (right) from Duke-NUS’ Health Services & Systems Research Programme have been focusing on understanding the pandemic’s implications on the healthcare system and population health
Swift isolation, quarantining and extensive contact tracing also played key roles in mitigating the outbreak. Isolation and quarantining may have their origins in the 14th century, but they remain among the most effective public health measures when dealing with a novel disease outbreak.
“From our computer modelling, it is very likely that if Singapore had not moved early and consistently to roll out contact tracing and quarantining and relied solely on treating infected individuals, the number of cases would have been much higher,” said Matchar, who is currently leading research into the effectiveness of public health interventions against COVID-19.
The power of a learning health system
While the system was well prepared against a virus like SARS, SARS-CoV-2’s ability to spread in some hosts even without causing symptoms brought with it new challenges. Fever screening measures were no longer enough to pick up everyone who carried the virus.
“This emphasises the need for us to approach things with a dynamic and open attitude,” said Ong.
Just as the prompt publication of the new virus’s genetic sequence enabled laboratories around the world to develop test kits that can identify the virus, access to live real-world clinical data was crucial for timely policy responses.
Throughout the pandemic, the Duke-NUS HSSR and SingHealth Health Services Research Centre teams of faculty, clinicians, data scientists, researchers and analysts were able to use live data from the emergency room, hospital system and even nation-wide sources to build their models. These models were originally set up to develop actionable insights into acute and chronic disease cases that were handled at the SingHealth Duke-NUS Academic Medical Centre.
“When the pandemic happened, our experts, who were already familiar with how the health system works, were able to engage and collaborate with hospitals, clinicians and others to formulate appropriate responses,” said Ong.
Analysing live data also enables health systems to avoid the pitfalls of fighting the last war. Having up-to-date information from the ground means care providers and governments can respond nimbly as more becomes known about the virus.
Turning to the indirect consequences of a pandemic
Unlike SARS, the impact of the COVID-19 pandemic will likely be measured in years. While Singapore’s healthcare system was well-equipped to manage the direct impact of COVID-19, researchers like Ong and Matchar are now studying the ripple effects.
“How to treat people with COVID-19 is just a piece of a larger puzzle. We have to think about the degree to which our responses to the pandemic can have rippling effects on other parts of our healthcare system in the long term,” said Matchar.
Among the responses that the team is studying is whether patients suffer negative consequences from delays in non-urgent surgeries, such as hip and knee replacements. Data from this study suggests that patients did not experience noticeable increases in serious complications from these delays.
“We still have to see what the longer-term consequences may be, such as continued difficulty walking because joint replacement was delayed, but what we’re not seeing, for the most part, is people coming back in with emergencies,” said Matchar.
It is these later waves that now occupy the HSSR team. These include the consequences from unmet healthcare needs and delays to chronic care, which bring new elements to existing projects. For example, in an existing project, the HSSR team is applying artificial intelligence to develop solutions that can reduce long-term complications for people living with one of the three Hs: hyperlipidaemia, hyperglycaemia and hypertension. With the COVID-19 pandemic, these solutions are being considered among a variety of strategies to optimise care in the face of reduced access to traditional services.
The other wave that the team is focusing on is the long-term distress caused by COVID-19 and the resulting restrictions.
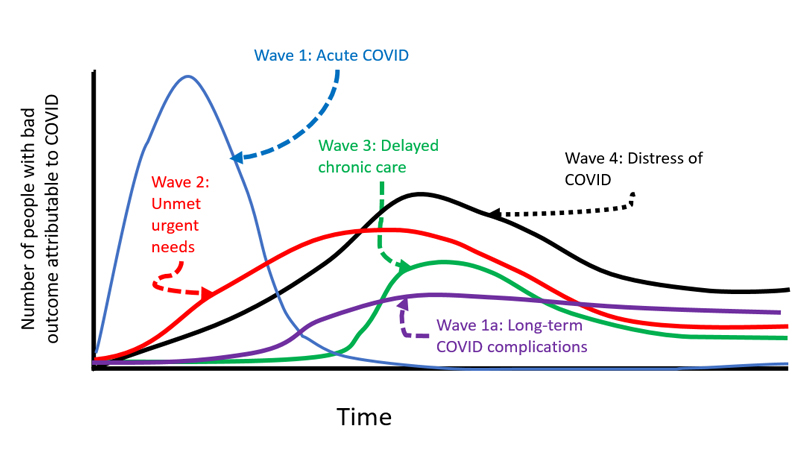
Duke-NUS scientists are studying not only the impact of the first wave of the pandemic but also the longer-term consequences
This causal diagram represents the reasons underlying the dynamics of the pandemic waves
“Stress and burnout and its manifestations can last months and perhaps years, so it’s that impact we’re trying to understand right now,” said Matchar.
While it will be impossible to predict the exact characteristics of the next pandemic, reviewing how existing and new interventions and innovations have worked is key to advancing preparedness. For example, being prepared to switch in-person follow-up appointments to teleconsultations, having resources available to support people who struggle with isolation and the mental stress on healthcare workers will make for an even more robust response.
“We will be much more prepared because all of those things that are now being thought of,” said Matchar.
What is clear is that as this pandemic stretches into years, its consequences will go deeper and further.
“We’ve just begun to scratch the surface of these indirect consequences,” said Ong. “Hopefully, when we have more answers and solutions to address them, we will be prepared for the next pandemic.”
As the knock-on effects of the COVID-19 outbreak ripple outwards, the spotlight has, for now, shifted away from Dr Ken Goh and the ICU teams. Following the intubation, Goh’s patient has recovered and went home.
Reflecting on those early days, Goh said that his team showed grit and focus despite the anxiety about facing an unknown threat: “We knew little then about the virus, such as the transmissibility and mortality rate of those infected. Many things were out of our control, so we needed to focus on preparing ourselves as best we could so that every patient would receive the best care possible.”