Mapping the body to understand the intricacies of human anatomy
By Dr Chua Li Min, Science writer
Clinical Assistant Professor Jai Prashanth Rao points out structures on a brain CT scan during a tutorial session
First-year medical student Ms Danielle Yap spends hours over her sketches, which she keeps in a book filled with illustrations of bodies and their intricate structures. Drawing is her way of consolidating what she has learnt during the cadaveric dissections in the wet lab as well as the virtual dissections on the Anatomage table.
“It helps me visualise the structures and integrate what I’ve learnt from my lessons with the resources available online,” added Yap.
“The wet labs were an invaluable resource as they help us understand anatomical structures in a more realistic sense beyond representations in textbooks,” added Yap’s classmate, Ms Devanshi Patidar from the Class of 2026. “Being able to physically feel and differentiate structures also gave us a lot more clarity.”
Rolled out 18 years ago, the “Normal Body” dissection course introduced by founding course director, Professor Pierce Chow has since evolved into the two-part “Foundations of Patient Care” course where students benefit from learning anatomy through more than just dissection in part 1 of the course.
A life-like sketch of the structures in the arm // Credit: Danielle Yap
With additional tools made available to students, they continue to learn the gross anatomy—structures of the body visible to the naked eye, alongside the physiology of the body while studying the appearance of different cell types under the microscope. All under the tutelage of a dedicated team of clinician-educators.
“Clinician-educators enable students to learn anatomy in a way that is useful to them as future would-be assistants to the surgeon in the operating theatre, through dissection following a surgical approach.”
Prof Pierce Chow
“Clinician-educators enable students to learn anatomy in a way that is useful to them as future would-be assistants to the surgeon in the operating theatre, through dissection following a surgical approach,” explained Chow, who is also a senior consultant surgeon at the National Cancer Centre Singapore and the Singapore General Hospital.
“Having them guide us (during the wet lab sessions) was a very good experience because it gave us a first-hand experience of how surgeons operate,” added Mr Sheriff Quek from the Class of 2026.
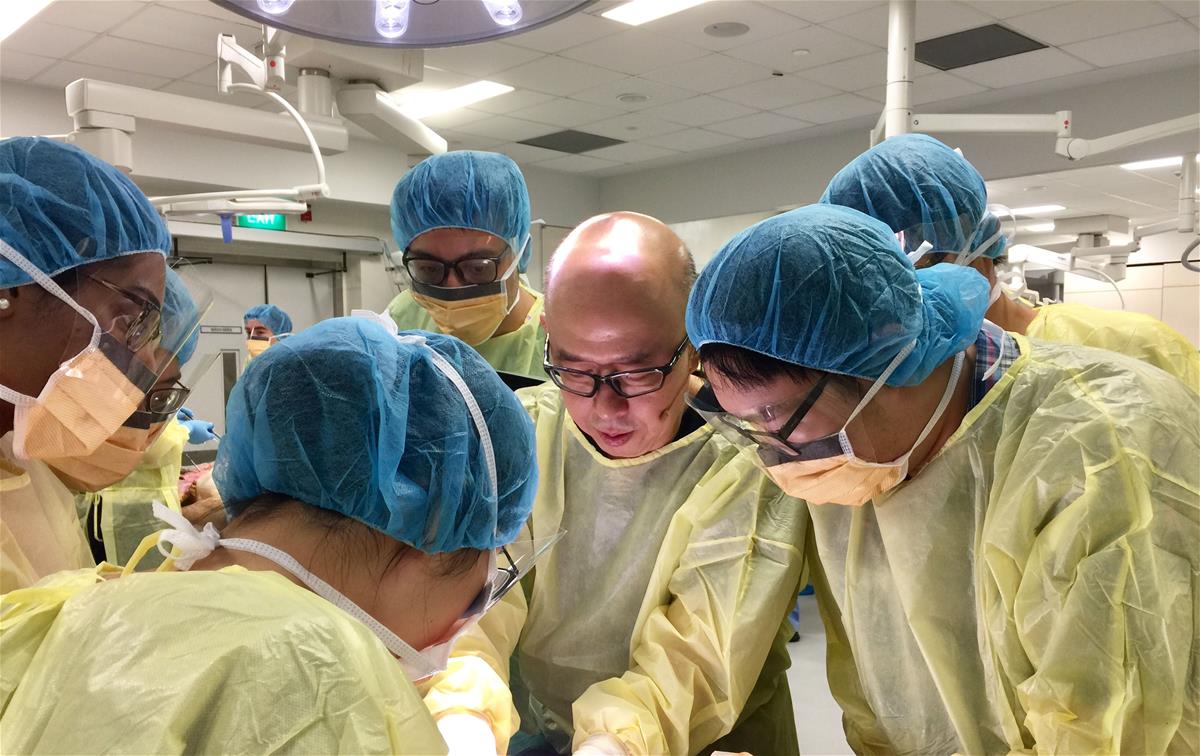
Professor Pierce Chow guides students during an anatomy class// Credit: Pierce Chow
Making a digital cut
Besides real human specimens and skeletons, students also explore human anatomy from different perspectives through a range of digital resources such as the Anatomage table, a virtual dissection tool that has been integrated into the 19-week long curriculum for students to review what they have learnt.
For the last teaching session of the block, the Class of 2026 was challenged to “treat” a 25-year-old man who was brought to the hospital after an accident. Their course instructor Clinical Assistant Professor Jai Rao set the scene for them: Though conscious and alert, the patient had come in complaining of severe headaches.
“When you are doctors, these are the types of cases that you see,” Rao, a practising neurosurgeon at the National Neuroscience Institute, reminded the class.
As soon as the patient’s anonymised CT scans appeared on the life-sized screen of the Anatomage, the students started talking through the case in their groups.
The silence of the Immersive Learning Space was interrupted by a deluge of questions and animated discussions among the students. Which region of the brain was affected? What symptoms would it cause? Should they be considering other conditions?
“It makes you think about the relevance of the patient’s history in his or her anatomy. And you can be a bit more focused and directed in your questions because you know where the problem is.”
Clin Asst Prof Jai Rao
“It makes you think about the relevance of the patient’s history in his or her anatomy. And you can be a bit more focused and directed in your questions because you know where the problem is,” said Rao, who is also with the SingHealth Duke-NUS Neuroscience Academic Clinical Programme. “You would also know what urgent conditions to rule out,” he added.
Toggling between the CT scan and the library of virtual brain cross-sections stored on the Anatomage, the students correlated the areas on the scan to anatomical structures.
“With the digitalised cadavers, students can do virtual dissection, they can easily access the whole library of cases to look at the related notes, imaging data and sometimes even the histology,” explained Associate Dean Professor Fernando Bello, who leads the Duke-NUS Technology Enhanced Learning and Innovation department.
His team has been working closely with educators like Rao, helping them to make the best use of technology in teaching anatomy.
After they were done, the students moved on to their next task for the day. In the Procedural Skills Learning Lab, they explored the anatomy of the brain again—this time in virtual reality, or VR. With a headset strapped on and controller in hand, the students were transported into the depths of the brain, where intricate vessels lie just an arm’s length away.
Working in pairs, they explored the brain up-close, finding their way around with the help of their partner.
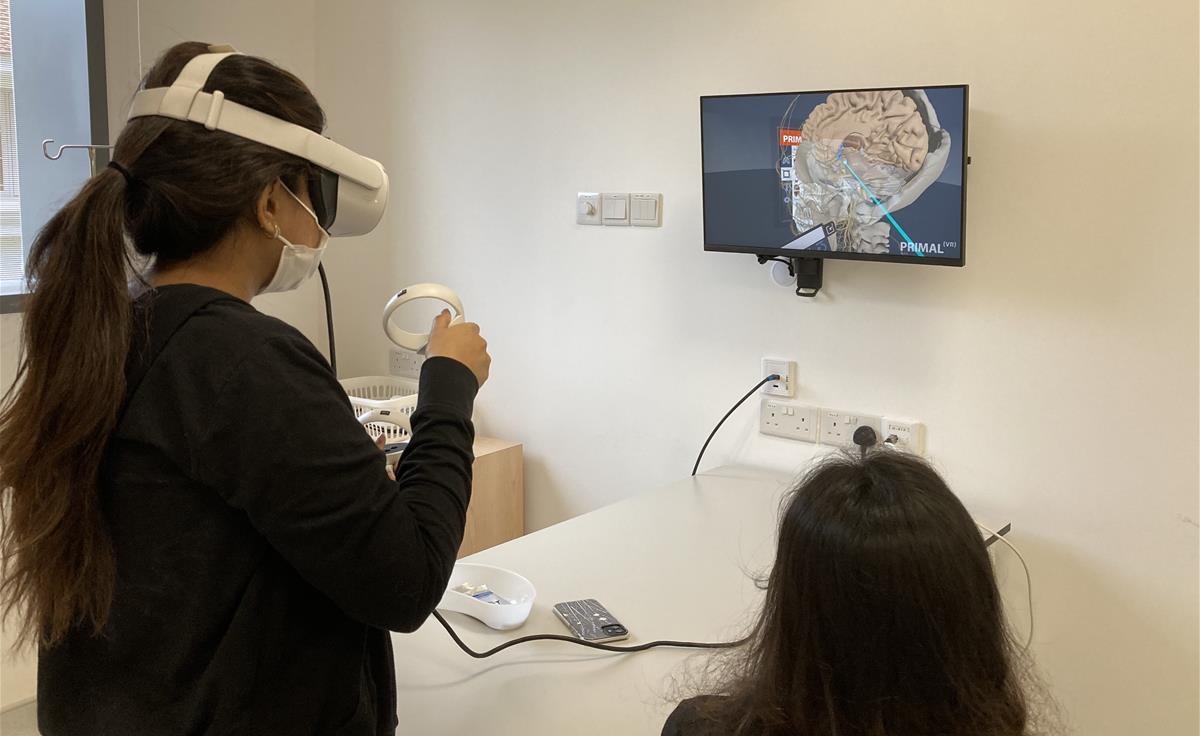
Students exploring the anatomy of the brain in a virtual reality setting
“I enjoy the collaborative nature of our lessons as we can work through cases together and teach one another,” said Devanshi.
“Our students find that it helps them connect what they’ve learnt so far while visualising it, so they enjoy that on top of the cadaveric dissections,” added Assistant Professor Irene Lee, who together with Clinical Assistant Professor Ignasius Jappar are co-directors of the “Foundations of Patient Care” course.
Getting acquainted with the technology
Ignasius remembers the first time he showed students the Anatomage. “It was the second day of their first week at School,” he said.
That afternoon, he performed a virtual dissection on the table, slicing into the brain of the digitalised cadaver, keeping the audience of 72 in the LEAD room enthralled by the different views of the brain.
To bring students and faculty up to speed with this new technology, the education team conducted several training sessions.
“One of the hardest parts was my own learning curve,” admitted Rao, who has been teaching neuroanatomy for the past 12 years. “I spent many many hours exploring the Anatomage, as well as the VR headset to understand the limits—and opportunities—of the systems.”
That made him realise the potential challenges that students could face.
Have a question? Send it in and it may be answered in the next issue of MEDICUS!
ASK MEDICUS
“If you’re too lost in that environment and the cognitive burden is too high, you’ll just not enjoy it and switch off,” added Rao, who also leads the neurosurgery residency training programme at SingHealth.
So he recorded annotated videos of himself performing digital dissections and navigating with the oculus, posting them as pre-reading resources for students.
“Once they are familiar with the technology, they actually move very quickly,” he observed. “It’s important that we don’t just put the technology there. You have to show the students how to use it and its relevance to what they are learning.”
So far, the results have been encouraging. “There was a lot more engagement and understanding and the level of questioning also went up,” said Rao.
Having these resources at their fingertips gives students the flexibility to plan their learning around the lessons, offering them the opportunity to revisit what they have learnt during cadaveric dissections, shared Yap and Quek.
Building a library of resources
In his days as a medical student at Duke-NUS, Ignasius and his peers from the Class of 2012 relied mainly on books and cadaveric dissection to learn about the gross anatomy of the body.
But the textbooks did not always have all the answers. “It was very difficult to navigate a lot of the anatomical structures that were often described in two or three pages in the textbooks,” said Ignasius.
Even though students could see and touch the structures during wet lab dissections, it was not possible to revisit certain topics or body systems after the lab sessions had concluded.
So the benefits of visualising structures on a software were immediately apparent to Ignasius. “When you view the same structure in the software, it is so much easier to flip and move it around. This enhances our understanding of the relative position of an organ to other systems,” he explained.
It also meant that students could access the online resources anytime, anywhere. But what if they could do more—like giving students the opportunity to access the physical structures anytime?
That was when the team ventured into the realm of 3D printing, which enables them to duplicate anatomical models. This semester, for example, students were given 3D-printed copies of vertebrae from different sections along the spine when they were learning about the musculoskeletal system.
“It gives us better visualisation than what the textbook provides, because it enables us to see the structures from a 3D perspective,” said Quek.
According to Bello, the process is relatively quick and a vertebrae from the spine can be printed and post-processed in less than three hours.
And the team plan to expand the resource to include other structures, as educationalist Irene Lee shared: “Printing more structures will give our students more opportunities to study certain structures up-close. It’s pretty cost-effective, and scalable too.”
To complement the 3D printer, a 3D scanner that captures objects at a high resolution was also brought in. With the scanner in place, the education team is now exploring other ways to enhance learning for students. Such as scanning the structures from patient cases or existing models and 3D printing them, said Ignasius.
Instead of scanning to print, Rao has other plans for the scanner.
He hopes to build a one-stop digital library of anatomical resources to enrich students’ understanding of the natural variations of the human body—the ones that he comes across during cadaveric dissections in the wet lab or even in the clinic.
Printing a heart from scratch
A blended approach
“We’re gradually moving towards a multi-modality approach, where we use a range of different methods, not just technologies, but different ways of teaching and learning”
Assoc Dean Prof Fernando Bello
“We’re gradually moving towards a multi-modality approach, where we use a range of different methods, not just technologies, but different ways of teaching and learning,” said Bello.
Such an approach is the way to go, as it caters to the learning needs of different students. “Some prefer touching a real specimen. Some, on the other hand, would prefer to look at 3D models and move it in the virtual space,” explained Ignasius.

Scanning structures in 3D using a handheld scanner
Which is why the education team continues to seek innovative and meaningful ways in which wet lab experiences can be augmented, or even be translated into immersive virtual learning experiences.
But only if the technology fits, stressed Bello: “We should be using the method because it supports our students, and because it has a number of advantages. So it’s not the technology per se.”
Looking back at her learning experience during the past semester, Yap is grateful to the education team for their support.
“They are very thoughtful in planning and allocating resources. By making different educational tools available to us, they make sure that none of us are left out.”
First-year MD student Ms Danielle Yap